Patientenerfahrungen

Frauen, die nach einer Thermografie im Rahmen einer regelmäßigen Brustuntersuchung oder aufgrund einer Mammographie oder einer klinischen Untersuchung Fragen stellten, berichteten über ihre Erfahrungen.
Weibliche Bewertungen von Thermografie
Frau # 1
Eine Frau, die Thermografie-Tests für Brustkrebs hatte, sagte, sie habe beschlossen, es zu tun, weil sie einen Freund hatte, der an Brustkrebs starb. Die Frau hatte keine Familiengeschichte mit Brustkrebs und entschied sich für den Infrarot-Digital-Imaging-Test. Sie war beeindruckt, weil es sich nicht um einen invasiven Test wie bei der Mammographie handelte und der ohne Strahlung auskam. Der Thermografie-Test zeigte eine Anomalie und der Frau wurde empfohlen, ein Mammogramm zu machen. Die Frau sagte, sie hätte das Mammogramm und eine MRT bereits machen lassen, die beide nichts zeigten. Dann machte man einen Ultraschall, der die Veränderung zeigte, die die Thermografie auswies. Sie ließ eine Exzisionsbiopsie (Herausschneiden des Befundes) des abnormalen präkanzerösen (Vorzeichen von Bösartigkeit) Gewebes und sagte, ohne die Thermographie wäre sie möglicherweise erst gefunden worden, wenn sie eine radikalere Behandlung wie eine mögliche Mastektomie benötigte.
Frau # 2
Diese Frau sagte, dass sie einen Schrecken hatte, nachdem sie einen Knoten gefunden hatte und ein hohes Risiko hätte, weil ihre Mutter an Brustkrebs starb und die Großmutter ebenfalls Brustkrebs hatte. Nach der Thermografie hatte sie am selben Tag die Ergebnisse.
Frau # 3
Diese Frau ließ jährlich eine Thermografie machen, nach dem Verlust ihrer 32-jährigen Tochter an Brustkrebs im Jahr 1999. Sie lässt bis heute nach der Thermografie einen Ultraschall folgen und versteht nicht, warum nicht jeder Arzt den Infrarot-Test zu den verwendeten Tests für jährliche Brustkrebsuntersuchungen hinzufügt.
Brustkrebsfälle
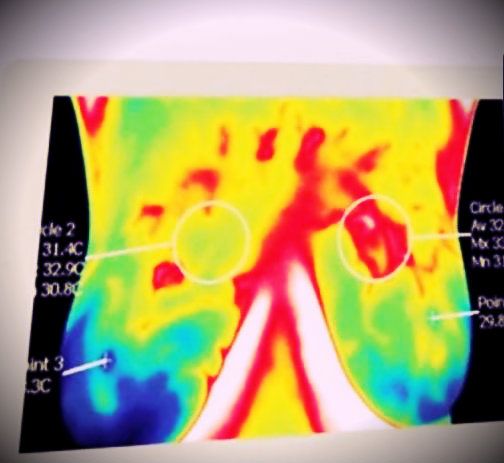
Die Frau hatte ein hohes Risiko für Brustkrebs sowie einige klinische Befunde. Sie hatte das Gefühl, dass Mammographien nicht signifikant genug waren und Thermografietests vorgeschlagen. Sie wusste, das sei nicht-invasiv und fühlte sich gut informiert. Man fand TH3-Gewebezellen (Th3-Zellen treten vermehrt in Gewebe mit erhöhter Antigenlast auf, wie im Tumorgewebe in der rechten Brust und normale TH1-Zellen der linken Brust). Ein Nachfolge-Thermogramm brachte sechs Monate später ähnliche Ergebnisse. Sie änderte ihre Ernährung auf vegetarisch, nahm Nahrungsergänzungsmittel, um das hormonelle Gleichgewicht zu unterstützen, und senkte ihre Östrogendosis. Der Test ein Jahr später zeigte beide Brüste mit normalen TH1-Zellen.
Heilungsrate von Brustkrebs
Die Heilungsrate von Brustkrebs im Frühstadium beträgt 96 % und mit Thermografie-Tests kann man sie mehrere Monate auseinander halten, weil es keinen Strahlungsfaktor gibt. Risikofaktoren lassen sich mit modifizierten Diäten, Östrogensenkung und Veränderungen des Lebensstils senken, um drastische Maßnahmen zu vermeiden. Die Thermografie findet 10 % mehr als Mammogramme oder Ultraschalluntersuchungen oder invasive Tests.